COVID Transmissions for 10-8-2021
Is Pfizer waning? Are antigen tests worthwhile? Let’s discuss.
Greetings from an undisclosed location in my apartment. Welcome to COVID Transmissions.
It has been 691 days since the first documented human case of COVID-19. In 691, the death of Frankish King Theuderic III makes his 9 year old son Clovis IV the sole King of the Franks. The end result of this is that Pepin of Herstal, his Mayor of the Palace, becomes the true ruler of the Franks. Pepin is the founder of a family that goes on to become the Carolingian dynasty of Frankish emperors.
Today we discuss vaccine effectiveness studies for the Pfizer vaccine, a hot topic lately. Also, we will discuss rapid antigen tests.
Have a great weekend!
Bolded terms are linked to the running newsletter glossary.
Keep COVID Transmissions growing by sharing it! Share the newsletter, not the virus. I love talking about science and explaining important concepts in human health, but I rely on all of you to grow the audience for this, which you can do by using this button here:
Now, let’s talk COVID.
New studies update evidence on Pfizer vaccine effectiveness and durability
Several new real-world evidence studies have been published regarding the Pfizer vaccine recently, and I’d like to walk through what we are looking at. The ones that have made it to my radar are two in the New England Journal of Medicine (NEJM) and one in The Lancet.
The first, an Israeli study, reports waning antibody levels over months following complete vaccination—this one in NEJM: https://www.nejm.org/doi/full/10.1056/NEJMoa2114583
This one is interesting—it doesn’t look at the effectiveness of the vaccine, but only at antibody levels. It makes a distinction between overall immunoglobulin (aka antibody molecules, or Ig) that recognize SARS-CoV-2 vs neutralizing antibodies that can surround and inactivate virus, rendering it unable to infect. The paper demonstrates a steady decline in overall anti-SARS-CoV-2 Ig, beginning about a month after the second vaccine dose is administered:
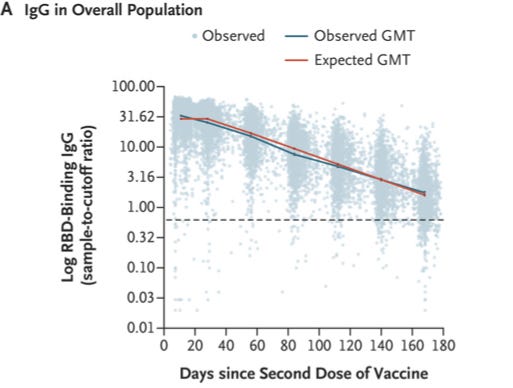
The thing about the data here is that they do not tell us much, directly, about what is going on with effectiveness of the vaccine. These antibodies are not directly responsible for protection against COVID-19, though it is interesting that they wane. Also, it is not terribly surprising that antibodies overall wane after vaccination. The immune system spends time maturing and pruning back less-relevant response over the time after it sees an antigen. Also, without an active infection, there is less need to be churning out antibodies. Levels decline as result of these things, and eventually they typically reach a steady state. For this reason, it can be challenging to use widely-available antibody tests as a means of measuring protection. They don’t really tell you what the level of neutralizing antibody really is, and neutralizing antibody is what you really want to measure, but what’s more, low levels do not necessarily mean you don’t have a memory response that can spring into action.
Now, this paper also looked at the neutralizing antibody level over time:
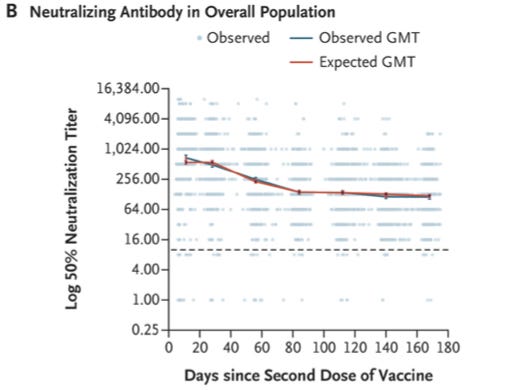
These data are more like what I might expect; we see that after vaccination is complete, the antibody levels do begin to fall. However, they reach a steady state, again something that we would expect when a solid memory response is generated.
Especially interesting here is that the neutralizing antibody study here is done in a population that is actually a subset of the overall antibody study. In this subgroup, there was a high proportion of people with coexisting medical conditions and older persons. We would expect responses to be less robust and less durable in this group, but here they look to be both robust and durable.
I’ve seen this study reported as providing evidence of vaccine “waning,” but I honestly don’t see that here. While we know that there is some drop over time in protection against specific disease outcomes in specific populations with this vaccine in particular, I don’t know that these are explained by the data that we observe here. There are simply too many unknowns in human behavior, and it does appear from these data that neutralizing antibodies, which are what we think are correlated with protection, level off and stay stable.
Now, look, a lot of what I’m saying here is meant to address what I’ve seen in the press out of this paper, but there is something I want to mention—this paper is super valuable. The authors made an effort to correlate antibody levels overall with neutralizing antibody levels. That is a really good move, because it is a lot easier to measure overall antibody levels than it is to do the assays necessary to determine neutralizing antibody titers. With a correlation, it may be possible for those widely-available antibody tests to tell us something meaningful about protection. However, since the two things change over time in different patterns, I’m not sure how usable it will really be. We’ll see more on that later, I think.
On to the second paper—this one is also from NEJM but looks at vaccine effectiveness in Qatar, where there is a high rate of uptake of the Pfizer vaccine: https://www.nejm.org/doi/full/10.1056/NEJMoa2114114
This is a straightforward paper looking at vaccine effectiveness over time. It tells us that in the real-world population, effectiveness against any infection with SARS-CoV-2 peaked at 77.5% one month after full vaccination was completed. After that, it waned over the next 5 to 7 months, reaching a low of 20%. Unfortunately, the picture looks similar for effectiveness against any symptomatic disease, which was the original endpoint in the clinical trials. That said, effectiveness against severe, critical, or fatal cases of COVID-19 reached 96% and stayed there.
In this instance, I am pretty convinced that we are seeing a meaningful decline in the effectiveness of the Pfizer vaccine against mild or asymptomatic disease. The reasons for this could be a combination of factors, and I think it’s important to be aware of that. In the original clinical trials, participants were studied in the context of COVID-19 control restrictions that were put in place for a world without any vaccines. These were severe, as we’ll all remember, and may have impacted the opportunities for virus transmission events to take place in the trials. Now we are looking at real-world data from a situation where people feel confident with vaccination and may have acted with greater laxity. I expect this contributed somewhat to the effects being seen here, but I don’t expect that it represents the entirety of the effect. The other comment I want to make is that this study applies in Qatar. It is not necessarily generalizable to global experience, as we will soon see. Still, it says something.
The reality is, it looks like it’s more possible to get sick with COVID-19 again, albeit mildly or with no symptoms at all, for a vaccinated person about 6 months out from their second dose. That said, such a person is in a lot less trouble than they would have been without their vaccination, and unlikely to end up with severe disease or in a hospital.
My takeaway here is that it’s worth continuing to take some precautions if you’re vaccinated, but we knew that. You might eventually get COVID-19—in fact, many of us probably will—but the result is very likely to be a mild illness if you are vaccinated, one which will reinforce your immunity and keep you out of the hospital.
Now on to the final study of this trilogy. This one is a study on the US experience of the Pfizer vaccine, in The Lancet: https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(21)02183-8/fulltext
Overall effectiveness against infection with SARS-CoV-2 was 73%, but this represents a trend with change over time. It began at 88%, but by 5 months after full vaccination it had fallen to 47%. Lest we think that this was mostly because the Delta variant changed the game, they did some sub-analyses showing that early after vaccination, effectiveness against Delta was over 90% but dropped to 53% by month 4 after vaccination. For older variants, it started at 97% but dropped to 67% 4-5 months after vaccination was completed. So, there is a general trend of loss of effectiveness against infection. The difference in rate of decline between variants was not statistically significant.
I’ll remind, of course, that vaccination was originally studied against symptomatic disease, not infection overall. If you get infected and you don’t get sick—but you might have otherwise—that’s the vaccine doing its job. So I might not be using that endpoint the way all these studies are doing. But, I’m not in charge.
Looking at something that really tells us about impact on disease, effectiveness was 93% against hospitalization or death and it stayed stable there.
This is a less dire study than the one out of Qatar, but it brings me to the same conclusion: a vaccinated person still needs to be careful, but is not likely to get severe disease and when they do eventually get COVID-19 they will be protected from its worst outcomes.
Taking these three studies together, we know that the Pfizer vaccine produces a stable neutralizing antibody response that protects against severe disease excellently while offering reasonable, but slightly waning protection, against more mild manifestations of infection. This latter pattern might be mitigated with boosters, but on the whole I am not overly concerned about the situation. As long as we stay responsible about our behavior, I still think everyone who got this vaccine is excellently protected.
Biden administration invests $1 billion in rapid antigen tests
The US is behind the curve when it comes to rapid, at-home antigen tests that can be used on a daily basis to check for infection. These tests are great. They are not as sensitive as a PCR based test, but they are excellent at detecting infections that are able to transmit to other people.
These tests should be used on a daily basis, so that if they do miss an active infection one day, they might catch it the next. The nice thing about them is that they are cheap, so they can very much be used on a daily basis. Except in the US, where they remain expensive and scarce. To mitigate this, the Biden administration is working on investment in rapid antigen tests to make them more available in the US. You can read about it here: https://www.washingtonpost.com/health/2021/10/06/biden-rapid-at-home-covid-tests/
Thing is, this is not nearly enough money invested. One billion dollars? The US spends 600 million a year on basic office supplies. This is only a little more than that, and on a priority that is mission-critical to fighting the pandemic. Don’t get me wrong, I’d rather see this investment than not, but it should be ten times as high. I want a world where these tests cost $5 for a whole week’s worth. We need to get there.
What am I doing to cope with the pandemic? This:
Watching: Ted Lasso
Look, this show just won 4 Emmy awards, and it earned them. It is actually worth getting Apple TV to watch this. It is refreshing and uplifting and displays a model of masculinity that is optimistic and non-toxic. I strongly recommend it.
You might have some questions or comments! Send them in. As several folks have figured out, you can also email me if you have a comment that you don’t want to share with the whole group.
Join the conversation, and what you say will impact what I talk about in the next issue.
Also, let me know any other thoughts you might have about the newsletter. I’d like to make sure you’re getting what you want out of this.
Part of science is identifying and correcting errors. If you find a mistake, please tell me about it.
Though I can’t correct the emailed version after it has been sent, I do update the online post of the newsletter every time a mistake is brought to my attention.
No corrections since last issue.
See you all next time. And don’t forget to share the newsletter if you liked it.
Always,
JS







A couple of weeks ago, didn't Johnson and Johnson release data indicating that their vaccine shows no waning at all after six months? (That was the one-dose original regimen. Presumably the two-dose version would last even longer.)